Paper based medical records - the elephant in the room
 Healthcare associated infection can be one of the biggest challenges faced by a health care facility.
Healthcare associated infection can be one of the biggest challenges faced by a health care facility.
The NHMRC in their report ‘Australian Guidelines for the Prevention and Control of Infection in Healthcare (2010) stated that ’There are around 200,000 healthcare-associated infections (HAIs) in Australian acute healthcare facilities each year. This makes HAIs the most common complication affecting patients in hospital.’
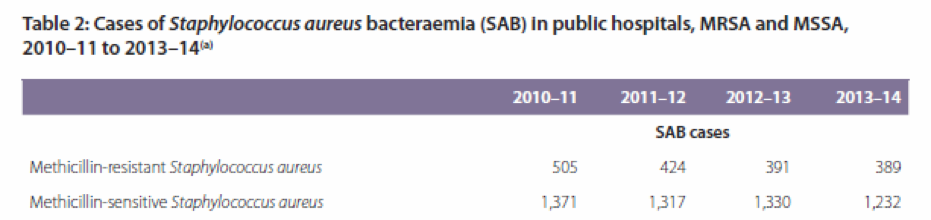
The AIHW in their report ‘Staphylococcus aureus bacteraemia in Australian public hospitals 2013–14’ found that 1,621 of these HAI’s were attributable to Staphylococcus aureus bacteraemia (SAB) or ‘Golden Staph’.
The report found however that the overall number of reported cases had decreased from 1876 in 2010 to 1621 in 2013-14.
Australian Infection Control Initiatives
While the decrease in SAB’s is certainly good news, the rate of HAI’s overall is still exceptionally high.
Many initiatives have been put in place in an effort to reduce the number including:
- National Safety and quality Health Service Standards (NSQHS)
- National Infection Control Guidelines
- National Standard definitions for measurement
- National Hand Hygiene Initiative
- Antimicrobial Stewardship Clinical Care Standard
No doubt these initiatives are great news, and health care institutions go to great lengths to ensure adherence to these standards, but perhaps there may an elephant in the room that hasn’t been considered.
Paper Based Patient Charts

As supposed to digital patient charts, traditional paper based medical charts and records are constructed from…well paper. Being made of cellulose, paper has a fibrous texture capable of absorbing bodily fluids such as blood and other human secretions. Viewed under a microscope, an ordinary piece of paper looks like the image to the right.
Infectious diseases – even common ones such as viral conjunctivitis – are spread rapidly through touch, air, bodily fluids and soiled objects.
Paper charts and medical records are made from absorbent paper, which can aid in the transfer of pathogens from patient-to-practitioner or patient-to-patient. Think about it; in a situation where a doctor leaves a room having seen an infectious disease, there is a protocol in place that means the room is wiped clean of pathogens. The operating table, chinrests, armrests, door handles – all are wiped down with alcohol wipes. All except the paper chart that is.
Wherever the patient goes, the chart goes.
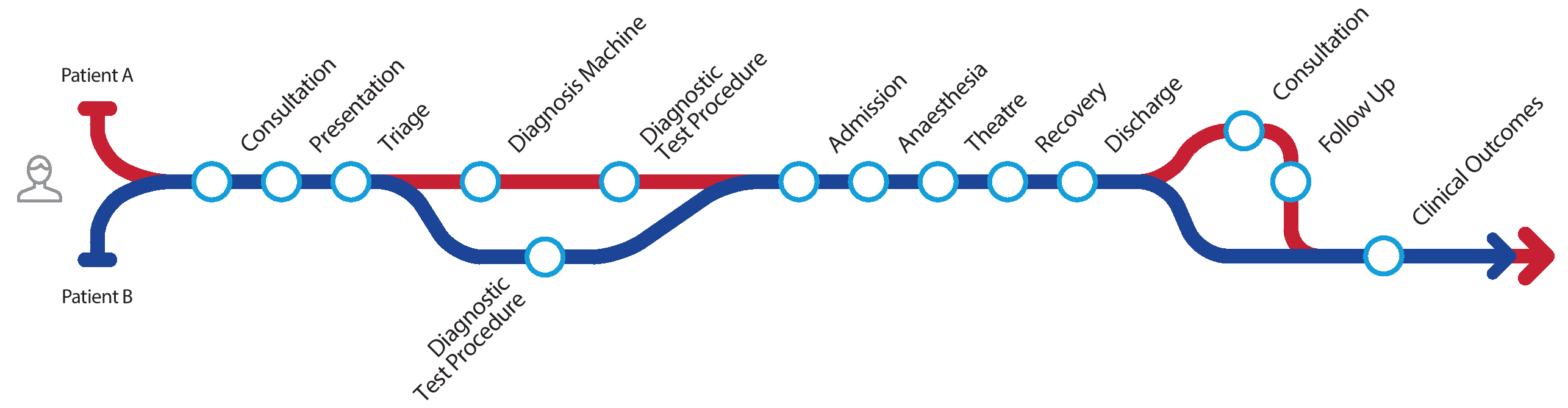
The diagram above shows a typical patient care pathway. As the patient travels through each care event, so does their chart. The patient chart is opened and inspected, added to and closed in every area of care. It goes through many care givers' hands.
The problem becomes more significant once the patient arrives at an area such as theatre where the chart may become exposed to a procedure or treatment resulting in the exposure of blood, secretion or other bodily fluids.
The chart is opened and inspected, added to and closed by a clinician performing or assisting in the procedure.
The Chart then goes to Recovery, the patient is discharged and the chart finds its way back in the hands of an administrator who completes the coding and billing and then stores the chart.
While the care givers wear gloves when they handle the chart, administrators do not.
Given this, the potential for cross contamination across charts (and patients, and staff) as they change through hands must be considered a possibility.
It certainly something that should be considered in strategies to reduce HAI’s.
Are Paperless Patient Charts the Answer?


![How to transition to paperless medical records systems. [3 Tips]](https://blog.scancare.com.au/hubfs/lady_photocopying.jpg)